
For most of her life, Napolo from Narok County, Kenya suffered from eye pain. The 78-year-old first noticed the discomfort when she was in her thirties. She said it felt like there was always sand in her eyes.
Then her eyelids started turning inwards, causing more pain and irritation. She tried traditional remedies like plucking her eyelashes, but nothing helped. Her vision worsened over time.
One day, a community health worker came to Napolo’s doorstep to check on the family’s vision. Thanks to the primary eye care training we’d provided, the community health worker took one look at Napolo’s eyes and instantly knew what the problem was – a trachoma infection.
Trachoma is a bacterial eye disease that is a leading cause of blindness in areas with water shortages and crowded living conditions. The infection spreads easily through hands and clothing, and also through direct transmission by flies. If left untreated, trachoma forces the eyelid inward – like Napolo’s – making the eyelashes rub painfully against the cornea. Over years, it can lead to permanent scarring and irreversible vision loss.
The community health worker helped connect Napolo to our partner hospital for treatment. As Napolo was in the late stage of the disease, she required surgery. At our partner facility, the Talek Health Centre, she underwent an operation that corrected her inward-turned eyelids. The procedure brought her immense relief and preserved her remaining vision.
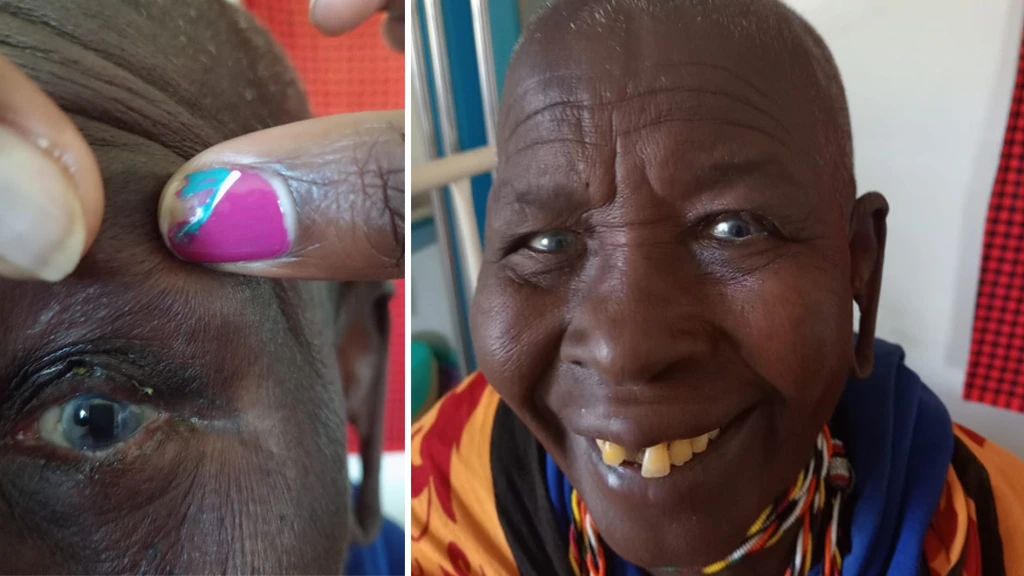
Stories like Napolo’s are an example of how we strive to address the root causes of avoidable blindness through a disease control approach. Our model helps us diagnose, treat and prevent the major causes of vision loss, including cataract, diabetic retinopathy, glaucoma, trachoma and uncorrected refractive error.
Throughout Kenya, Ethiopia and Zambia, we’ve been working with communities and partners to eliminate trachoma through a four-step approach known as SAFE.
The SAFE acronym stands for:
In Kenya, we work with government partners to distribute antibiotics to regions where trachoma is endemic. These antibiotics help prevent infection and can help clear up existing infections.

And because trachoma spreads quickly in areas where water is scarce, part of our approach is to make sure that people in our partner communities have access to a clean water source – by repairing and drilling water boreholes.
In the past couple years, we’ve focussed on training groups of local volunteers – called “Area Pump Minders” – in hand pump maintenance. That way, when a village borehole breaks down, someone in a nearby community will be around to fix it quickly. Throughout 2024, we hired on some of the Area Pump Minders we’d already trained to repair 129 boreholes – benefiting the nearly 130,000 thousand community members who depend on them.
Glaucoma is a tricky condition that often goes unnoticed until the damage is already done. Caused by increased pressure within the eye, it affects the optic nerve at the back of the eye, resulting in loss of nerve function and peripheral vision.
This often occurs painlessly, making it hard to detect. And any vision loss caused is generally considered irreversible. But if glaucoma is diagnosed early enough, it can be treated and managed with eye drops and medication, as well as regular checkups.
Ayetu, a farmer in Ghana’s Central Region, first noticed that he was having problems with his vision several years ago. After visiting the hospital, where he got a diagnosis of glaucoma, he started using eye drops. But finances were tight, and he found it difficult to pay for the medicine and attend his monthly appointments. Eventually he gave up and turned to herbal remedies, and when he did, his vision worsened.

In 2022, we started a community health project with the Winneba Municipal Hospital. Glaucoma patients with financial difficulties, like Ayetu, were told that their medication and appointments would be given free of charge – thanks to the generosity of donors.
When Ayetu found out he could get his medication once again, he felt enormous relief. He had worried about going totally blind, leaving his 75-year-old wife to manage the household on her own. Now, he says that the pain and tearing in his eyes has ceased, and the pressure has stabilized. “I was overwhelmed with gratitude when I started receiving these medications every month,” he says.
Today, little Ayan and Vyan in India have a bright future ahead of them – but as infants, these twin girls narrowly escaped a life of blindness.
Born two months early in June 2022, the girls weighed just three pounds each and suffered from lung infections. They were rushed to a nearby Neonatal Intensive Care Unit (NICU) in their city of Moradabad where they were stabilized. While there, the doctor treating the girls recommended that they undergo screening for Retinopathy of Prematurity, also known as ROP.
Retinopathy of Prematurity, as the name suggests, is a condition that can occur in preterm and low-birth-weight babies. It causes abnormal growth of the blood vessels that attach to the retina, which leads to later vision loss if left untreated. It’s difficult to detect, and in the worst case scenario it can cause a child to go suddenly, irreversibly blind.
Since 2022, we’ve been working closely with our partners at the C. L. Gupta Eye Institute to screen and treat preterm infants throughout Moradabad and its surrounding districts for ROP. The Retinopathy of Prematurity Eradication Project runs a fully-equipped mobile screening van. A highly trained optometrist makes rounds of all the local NICUs, screening babies for ROP, treating simple cases and referring more complex cases back to the base hospital.

Little Ayan and Vyan underwent screening, and both were diagnosed with severe ROP. At just five weeks old, they underwent eye injections, followed by laser treatment. Now, thanks to regular checkups, their condition has been addressed, and the little girls can live up to their full potential with their vision intact.
These twin girls are just two of many infants that have benefited from increased ROP screening in their community. In 2024, we expanded the program to 28 NICUs in five districts across the region, enabling us to screen an additional 1,500 infants for ROP and provide treatment for 400 of them.
At just eight years old, Fassikaw in Bahir Dar, Ethiopia decided he’d had enough of school. His eyes were always watery, he couldn’t read the blackboard, he had to hold books just inches from his face and his grades were suffering as a result. He told his parents he wanted to quit.
His parents didn’t let him leave school, and when they heard about a school eye health program that was offering free diagnosis and eyeglasses to students, they jumped at the chance. They took Fassikaw to our partner hospital where they learned that he needed strong corrective glasses. Thanks to Partners in Education Ethiopia and our generous donors, he received the eyeglasses at no cost. Now that he can see, Fassikaw is finding school much more engaging, and his grades are on the rise.

What the little boy probably doesn’t know is that vision impairment like his prevents a lot of children around the world from finishing their schooling. In fact, children with vision loss are up to five times less likely to be enrolled in formal education in low-and middle-income countries, and a pair of glasses can reduce the odds of failing a class by as much as 44 per cent.
That’s why we help run school eye health programs, reaching children right where they need vision care the most – in the classroom. By training teachers and school health coordinators in primary eye care, we’re able to screen thousands of students in just days, quickly identifying those with possible vision loss for further referral. That way we can help more students like Fassikaw stay in school and thrive in life.
Adults, of course, also suffer from refractive errors, and sometimes providing a pair of reading glasses or prescription eyeglasses can change the course for an entire family. Take Junmoni’s story as an example. The mother of two in India helped support her family’s income by doing handloom weaving from her home. But as she got into her forties, she found it harder and harder to see the intricate patterns she was weaving. In despair, she was readying herself to sell off her handloom when she was surprised one day by a knock on the door. A visiting community health worker did a quick vision screening test and told Junmoni she likely just needed a pair of glasses. With a referral in hand, Junmoni visited one of our eye screening camps where she got a diagnosis and a pair of prescription bifocals all free of charge. Now she’s weaving again and saving up so she can send her young daughter to college.

We can provide eyeglasses to people like Junmoni and Fassikaw, with all associated expenses, for about $20 dollars apiece. In 2024, we distributed more than 270,000 pairs of eyeglasses – that’s a lot of lives transformed.
Across the world, more than 17 million people are blind due to cataracts, and cataracts cause another 34 million people moderate to severe vision impairment. But they are easily treated. A simple day surgery, one per eye – at the cost of about $75 Canadian dollars – can restore vision.
Despite that, millions around the world aren’t getting the surgery they need. The barriers are innumerable but usually include lack of financial resources to pay for the surgery, and lack of transportation to access the healthcare system. That’s why we work in rural, remote and underserved communities, identifying eye conditions like cataracts on people’s doorsteps and connecting them to the healthcare system – then ensuring that their treatments and transportation are subsidized or provided free of charge.
For someone like 85-year-old Esther in Kenya, a visit from a community health promoter made all the difference. Living in the remote village of Sitet, Esther struggled to get together the money just to visit the nearest hospital, let alone pay for the appointment.
About 10 years ago, when Esther was chopping wood, a log bounced up and hit her in the left eye. The pain was extreme, but she decided to wait and see what happened. A week later, in unbearable pain, she travelled to the hospital for help. There she received pain medication and a referral to an eye hospital. But by then, she was out of money. She went home and the vision in her left eye never recovered.
Three years ago, she started to notice the vision in her right eye was also fading. Soon, she could no longer manage her household, and her daughter had to move in with her.
“She had to leave her home to stay with me and help,” says Esther, about her daughter. “At some point, I just wanted to die… I didn’t want to hold her back from her life.”

One day, hope arrived in the form of a community health promoter who knocked on Esther’s door. The health promoter referred her to an eye screening camp, where she was diagnosed and referred for cataract surgery on her right eye. Unfortunately, the damage to her left eye was irreversible, making treatment of her right eye even more essential. As part of our program, Esther’s transportation, appointments and surgeries were all paid for, thanks to the generosity of our donors and partner, Johnson & Johnson.
Today, Esther is back to living independently – visiting friends, walking to church and picking and drying her own coffee beans.
Every year, the community health workers we train bring hope to thousands of seniors like Esther who once believed blindness was inevitable. In 2024 alone, community health workers helped us restore sight by making referrals for more than 230,000 cataract surgeries – giving people back their independence and dignity.
Seeing care through to the end
Our model offers patients the full continuum of care – from screening and diagnosis, through treatment, to follow-up. After surgery, our teams make home visits to check on healing, answer questions and make sure patients attend follow-up appointments. This helps us troubleshoot issues early and keep recovery on track.
For cataract patients, follow-up is especially important. When someone has cataracts in both eyes, we often schedule surgeries several weeks apart. That gap gives time for healing and reassessment, because the outcome of the first surgery can guide the second.
Eye surgery changes lives, but recovery looks different for everyone. By staying with patients through every step, we prevent complications, improve outcomes and build trust. When communities know we’re here for the long haul it makes our work more sustainable, with healthier futures for all.
Vision loss doesn’t have to be inevitable. From Napolo in Kenya to Ayetu in Ghana and little Ayan and Vyan in India, these stories remind us that blindness can often be prevented or treated when care is accessible. Through community outreach, early diagnosis and partnerships that remove the financial and geographic barriers, we’re restoring sight and transforming lives. But the need is still great. Millions of people remain at risk simply because they lack access to basic eye care. Together – with continued support and collaboration – we can ensure that no one is left in the dark. Donate today to help us in our mission to prevent blindness and restore sight.
Twelve-year-old Premi, in Rajasthan, India, loves reading and going to school, but in recent years, her enthusiasm for learning came under threat when her eyesight started to fade, making it difficult for her to read the blackboard and keep up with her studies.
Premi is one of three children. Her parents and older brother work as day labourers on nearby farms to support the family. Despite their efforts, money is often tight, and a visit to the optometrist would be a stretch for them. Fortunately for Premi, her school was visited by one of our eye screening teams as part of our Vision-centre Based Community Eye Health Project with our partner in the area, the Alakh Mayan Mandir Eye Hospital. Premi was quickly diagnosed with refractive error and received a pair of prescription eyeglasses, free of charge.
The whole family is grateful that this bright young girl can continue her studies, with hope for a brighter future.
Our approach to eye health ensures entire communities – including schoolkids like Premi – get screened for eye conditions and can access treatment at low or no cost. By offering multiple screening opportunities at schools, vision centres, screening camps and right on people’s doorsteps, we make sure nobody falls between the cracks.
Our approach starts at the planning level – working with government and community partners to select a location with a high prevalence of vision loss and low socio-economic status – and a partner hospital with a compatible mission and vision.
Next, we collaborate with partners on an action plan, define the project area and decide on locations for vision centres. Once established, the vision centres act as links between communities and hospitals, providing comprehensive eye exams, dispensing glasses and making referrals to our partner hospital for surgeries.
Then, the training of community health workers begins. These frontline workers, mostly women, learn how to conduct visual acuity tests, identify various eye conditions, make referrals and provide eye health education. For many of our beneficiaries, the relationship with our programs begins and ends with the community health worker – who might visit the same household many times, offering kindness, compassion and counselling to nervous patients, as well as their eye health expertise.

After their training, the community health workers fan out to our various communities of work, doing a baseline door-to-door survey and referring patients to the vision centres and partner hospitals for further diagnosis and treatment.
As we continue our work in the area, our teams organize various screening camps and school screenings to give everyone multiple opportunities to have their eyes checked. Community health workers also continue their door-to-door work, checking in on patients, providing eye health education and troubleshooting any problems patients might face in getting treatment. Teams crunch numbers to monitor progress and evaluate each project, later bringing in external agencies to audit the work.

When the community health volunteers have done their final survey to make sure there are no backlog cases, villages and communities are declared as Avoidable Blindness-Free through public celebrations. At this point, the vision centres have become self-sustaining, so they can continue to deliver quality eye care services beyond the project’s duration.
The community health workers we employ for our door-to-door surveys can offer much more than just eye health expertise. Many have received additional training in primary health care and can provide advice and referrals for things like immunizations, vitamins, and maternal and newborn health care.

Shakuntala, an Accredited Social Health Activist (ASHA) with the Government of India, spent eight years providing advice to expectant mothers, and offering newborn care support, before she received additional training in primary eye care. With her experience, she can continue to offer referrals and education to mothers while she does her eye health screenings.
In 2024 alone, our community health workers linked more than 50,000 children aged five and under with crucial vitamin A injections, which reduces the severity of childhood illness and increases survival rates, while also helping them develop healthy vision. Also in 2024, we referred more than 16,000 expectant mothers and 12,000 nursing mothers with health facilities for check-ups.
Moreover, a community health workers frequent visits to a household can help them monitor a patient’s progress not only with an eye condition but with other health problems as well.
Take Bulal in Nepal, for example, a 97-year-old man who has cataracts as well as diabetes. When Meena, an Operation Eyesight-trained community health worker, met Bulal during a door-to-door survey in 2021, she realized that he would need additional support to get the treatment he needed for his low vision. While he had been previously diagnosed with cataracts, the doctor told Bulal that his unstable blood sugar levels – and his high blood pressure – made cataract surgery too risky. Bulal thought he would live out his final days in darkness.

But when Meena heard his story, she set a plan in motion. Over the next few months, with Meena’s support and guidance, Bulal stabilized his sugar levels and brought down his blood pressure so he could safely undergo surgery. His family was grateful to see Bulal restored to his former dignity and independence once he could see clearly again.
From patient to ambassador – spreading the word about eye health
Ntiiti, a mother of five from a remote village in Kenya’s Kajiado County, started losing her vision in 2020. She didn’t know why she couldn’t see clearly and wondered if she was the victim of a curse. Soon, her vision was so poor that she could no longer perform essential day-to-day tasks like making meals, taking care of her children and looking after the family’s cattle.
Help arrived unexpectedly when a community health promoter, whom we’d trained in primary eye care, visited her home while conducting door-to-door screenings. He identified cataracts and sent her to a nearby eye screening camp for a formal diagnosis. At the camp, an ophthalmologist confirmed Ntiiti had bilateral cataracts and referred her for surgery. Ntiiti had never been to a hospital or clinic before, because of the distance to these facilities from her village, but our team helped arrange transportation so that she could get the treatment she needed. Thanks to our generous donors, she received surgeries on both eyes, free of charge.
Amazed by the difference the surgeries made to her life, Ntiiti told everyone in her community who complained of vision or eye problems about her miraculous recovery. Soon, she had her first recruit – a widowed mother of six who was living in total blindness. Ntiiti connected her to the community health promoter and even accompanied her to the hospital for her surgery.
We have many similar stories of patients like Ntiiti who become ambassadors for our programs. It speaks to the strength of our approach – by taking the time to build relationships in the community, patients with success stories become empowered to spread the word about the importance of getting treated for blindness and vision loss.

To create the biggest impact, we start at the community level. By training and empowering local health workers, we can help create lasting connections that bring eye care directly to people’s doorsteps. These trusted workers are the heart of our model – identifying problems early, guiding patients through treatment and spreading awareness that can transform entire villages.
With your support, we can train more health workers, open more vision centres and ensure that no one is left behind. Donate today to help us build a future where avoidable vision loss is eliminated for good.
Working as a nurse in a clinic in Ghana’s densely-populated Awutu Senya District, Joana Annobil treated a wide range of medical issues – from diabetes to hypertension. But there was one issue that consistently stood out to her as having the biggest impact on patients’ lives: vision loss.
“Our eyes are like the light of the human body,” she says. “Without your eyes, you can’t do anything. You can’t go anywhere. So, the eye is very important to talk about and take care of.”
Joana wanted to bring better eye health care to people in her district by studying ophthalmic nursing, but pursuing further studies felt out of reach because of the costs of leaving her job to attend classes full time. Still, Joana didn’t give up. After discussing her aspirations with the District Director of Health Services in Awutu Senya, our partner on a community eye health project, the director reached out to us for support. Thanks to the generosity of our donors, Joana’s dream became reality; we provided the financial assistance she needed to advance her education.

Today, Joana is fully certified as an ophthalmic nurse, after completing a degree program at the Korle Bu Teaching Hospital in Accra. She works at the Senya Beraku Polyclinic in her home district. She says that with her advanced training, she’s better able to diagnose, refer, and explain conditions and procedures to her patients. Most importantly, she is better equipped to combat eye health myths and misconceptions that prevent many patients from getting treatment.
Joana is just one of many healthcare providers and doctors whom we’ve supported in pursuing further studies since we were founded in 1963. One of the pillars of our work is to help build health systems by investing in hospital equipment and infrastructure, by establishing vision centres and by providing training opportunities for healthcare professionals. It’s all part of our sustainable approach to health care, which emphasizes building expertise at the local level.
The town of Chitipa is located at the northern tip of Malawi, hours away from the larger cities in the country’s more populous south. Until recently, people in the area had to travel between 100 to 350 kilometres to get any kind of eye health care because the local hospital was over capacity.
In March 2025, all that changed when we partnered with the Malawi Ministry of Health to open the new Operation Eyesight Vision Centre at the Chitipa District Hospital. Today, the district’s 256,000 people can visit the clinic to get everything from a routine eye exam to cataract surgery.

For Lydia, who lives in a village just outside of Chitipa, the new vision centre arrived just in time. For years, she’d noticed tearing in her left eye. Eventually, it became uncontrollable. She tried reading glasses, eye drops, various medications… nothing worked. Finally, she went to the hospital in Chitipa for help. There, she was diagnosed with cataracts and referred for surgery in Mzuzu, more than six hours away. She put off the operation while she saved money for the travelling it would entail.
When the new Operation Eyesight Vision Centre opened, Lydia was thrilled to find out that she could get her surgery much closer to home. In August 2025, she underwent the operation on her left eye, free of charge. Today, she is enjoying a higher quality of life, with her left eye no longer tearing up – and improved vision overall.

The vision centre in Chitipa is just one of many facilities we’ve helped establish in recent years. In May 2025, we successfully handed over a new eye clinic at the Garbatulla Sub-County Hospital to the County of Isiolo in Kenya. The clinic was developed in partnership with the county government and the Kenya Ministry of Health, with funding from Johnson & Johnson. Also in 2025, we laid the foundation stone for the construction of the Secondary Eye Hospital in Yadgir, Karnataka, India, in collaboration with the Shri Guru Mahipatiraj Eye Bank and Research Foundation Trust.
On the banks of the Ramganga River in Uttar Pradesh, India, sprawls the city of Moradabad, home to our partner hospital, the C.L. Gupta Eye Institute. In recent years, we’ve been working closely with the institute’s Vice-Chairman, Dr. Ashi Khurana, to help some of the area’s smallest residents – premature babies.
India has the highest rate of preterm births in the world, and the emergence of more Neonatal Intensive Care Units (NICUs) has greatly improved the survival rate of premature infants. But as more of these preemies grow up, an alarming trend is developing – some of these children end up going blind.
The culprit is Retinopathy of Prematurity (ROP), a condition that causes problems with the development of the blood vessels in the baby’s eye. If untreated, it can cause permanent vision loss and even total blindness.

Dr. Khurana remembers first hearing about the problem when a local doctor approached her with concerns about the high number of local children who had gone blind due to ROP. The problem, they realized, was a lack of screening at the growing number of local NICUs.
In answer, Dr. Khurana and her team launched a pilot ROP program to screen Moradabad infants for the condition, which later expanded to include a partnership with Operation Eyesight. Dubbed the Retinopathy of Prematurity Eradication Project, the program runs a mobile eye clinic staffed by an optometrist who has training in ROP screening and laser treatment. The optometrist travels with specialized equipment to NICUs throughout the area, providing both screening and treatment, while referring more complex cases back to the C.L. Gupta Eye Institute.

With help from Rotary Club partners, we supplied the program with essential equipment, including an imaging system used to examine the baby’s retinas, and a specialized laser system that is the gold standard for treating ROP. We also helped the hospital with the purchase of a mobile screening van, and we participated in the creation of educational materials to make sure that both healthcare providers and families understood the risks of ROP.
In the second year of the project, the screening area expanded from one district to five, including 28 NICUs. Between July 2024 and March 2025, 685 preterm babies were screened for ROP, with 54 of them receiving laser surgery, and another 35 treated with intravitreal injections.
Thanks to the generosity of our donors, we often purchase and upgrade ophthalmic equipment to help our partners offer the highest quality care possible, just like we did with the ROP project. Throughout our decades of work, we’ve equipped everything from vision centres to highly specialized operating theatres. We’ve also provided various types of vehicles to transport patients from rugged, remote locations to hospital, and to serve as mobile screening units on wheels – like the one now being used to screen infants in the Moradabad area.

In addition to donating equipment, we are committed to ensuring sustainability by providing additional funding for equipment maintenance training. In 2024, Dumisani Jere from our partner facility, Mzuzu Central Hospital in Malawi, was sent to India’s Aravind Institute to do a one-month Ophthalmic Instruments Maintenance course. Since then, he has been providing support to eye clinics throughout our project areas in Malawi’s Northern Region.

Hospital strengthening is at the heart of our mission to create lasting change. By investing in infrastructure, equipping facilities and training local professionals, we help build resilient health systems that can deliver quality eye care for generations to come. From vision centres in Malawi to advanced neonatal screening programs in India, these initiatives ensure that care is accessible, sustainable and rooted in local expertise. Thanks to the support of our donors, we’re not just treating patients – we’re strengthening health systems and empowering communities to protect sight for the future.
Donate today to help strengthen more hospitals and train more ophthalmic staff – For All The World To See.
Every day, 10-year-old Benjamin in Kenya proudly leads his family’s goats out to graze, a chore that once seemed unthinkable, because from a young age, Benjamin was blind.
Benjamin lives with his parents and six siblings in the village of Olookitareti in Kajiado County. The family struggles financially; Benjamin’s father Joshua has a chronic illness, while his mother, who lives with a disability, does her best to manage their livestock herds while also caring for the children.

In 2023, a local disability advocacy group referred Benjamin to a special needs boarding school, where he learned to read braille. His parents were grateful that he would receive an education, but they still worried about his future.
The following year, a community health worker identified cataracts in Joshua’s eyes during a door-to-door screening and referred him to our surgical camp. He took Benjamin along, hoping for a diagnosis for the child as well.
At the camp, Benjamin was also diagnosed with cataracts and referred to our pediatric cataract camp happening at another facility. But on the day of the camp, he didn’t show up. The outreach team made calls to the family to track him down, but their calls went unanswered. Finally, our community health promoter located Benjamin at his school. She later discovered that the family had lost their phone.
Recognizing the urgency of Benjamin’s condition, our outreach team contacted the family’s close friend, Pastor Titus, who accompanied Benjamin to the surgical camp with the family’s blessing.

Thanks to the support of our partners and donors like you, Benjamin successfully underwent surgery and had his vision restored. Joshua also underwent surgery and can now see clearly.
Now, Benjamin attends a regular primary school, confidently tackling Grade I. He reads and writes with ease and loves to join soccer games with the other children in the village.
His parents are grateful that Benjamin can now live up to his full potential.
Written with files from Patrick Wainaina Muthii.
This holiday season, consider giving the Gift of Sight to transform lives for more children like Benjamin!
Every time one of our community health workers interacts with a family during a door-to-door eye heath survey, she starts to collect data: the number of people in the house, their visual acuity scores, referrals given… and the list goes on. It all goes into a database so we can analyze the information and offer the community the best services possible.
As an international development organization and registered charity, we live in a world of data. The numbers we collect help us evaluate our programs, find efficiencies, show our impact and so much more. Our data builds trust with partners and donors, and it is the bedrock of one of our five programming areas: research and advocacy.
Thanks to our reputation as an organization that collects reliable data, we are increasingly being called on to participate in a variety of studies, and to add valuable input into policy decisions throughout the globe. Our growing credibility has opened doors to exciting opportunities, including leading major studies that shape national health strategies.
When Operation Eyesight began talks with Ghana’s Ministry of Health in 2006, with an eye on expanding our services into that country, what quickly became apparent was a lack of the kind of baseline data that we need when building our programs. After more discussions, it was decided that gathering that information would be one of Operation Eyesight’s first tasks in the country. Working with government ministries, along with several other organizations, we led the country’s first-ever National Blindness and Visual Impairment study.
At the helm of the study was our Technical Advisor, Dr. Boateng Wiafe, a widely respected ophthalmologist known for his decades of work advancing sustainable eye care across Africa.

Dr. James Addy, a co-investigator on the study and the former head of eye care with Ghana Health Service, recalls the lack of data at the time.
“We realized that we had only about two or three – not many – eye indicators in the platform that actually generates data for the country,” he says. “And from that study, we realized that 0.74 per cent of the population are blind … And then we had 1.07 per cent of the population having severe visual impairment. And so, putting everything together, it was about 1.5 million people who actually have visual problems.”
Published in 2015, the study continues to be a vital resource.
“The blindness and visual impairment study has been the go-to document for the government itself and all other non-governmental organizations working as far as eye health is concerned to plan their programs,” says Ghana Country Director Emmanuel Kumah, adding that it also informed the development of Ghana’s national eye health policy.
Data from the study was instrumental in the creation of the National Cataract Outreach Program, which offers quality cataract services to people in difficult-to-reach areas. The study’s findings also helped attract social enterprise and charitable eyeglasses providers to the country by proving the need for low-cost vision wear. Today, we’re looking for partners to help us update the nationwide study, ensuring Ghana’s eye health programs continue to be built on solid, current data.
An important part of our work is bringing eye care closer to underserved communities, which means establishing vision centres and eye units in collaboration with our partner hospitals. These facilities offer comprehensive eye exams, dispense eyeglasses, offer various treatments and refer more complex cases to the partner hospital. Some of these clinics are built in remote, rural areas, while others are established in busy, densely populated urban areas.
One of our urban vision centres is in a bustling, low-income neighbourhood in Pune, Maharashtra, India. To get a stronger understanding of its benefit to the community, the vision centre was the subject of a study led by the Community for Eye Care Foundation and members of our team in India. Over the four years of the study, 44,000 people living in the area were surveyed at two intervals by community health workers to track their eye conditions and their eye care-seeking behaviours.

What they found is that the prevalence of blindness and visual impairment in the community was reduced by nearly 62 per cent over the four years. Women continued to have a higher prevalence of blindness, but the gender gap narrowed during that same time span. The study found that more women visited the vision centre than men, and that more people made themselves available for a repeat eye examination during the second door-to-door survey. The study’s authors attribute these changes to the gentle nudging of the community health workers through their door-to-door surveys, and the existence of a nearby vision centre served by a predominantly female staff.
Our own CEO, Kashinath Bhoosnurmath and former Program Manager Soumya Moosa (now a Teaching Assistant at the University of Southern Mississippi), were co-authors of the study, published in 2022 in the India Journal of Ophthalmology.
Our participation in health studies continues to grow, with Operation Eyesight on board to gather data in Kenya for a joint study, between the London School of Hygiene & Tropical Medicine and other partners, that’s investigating the economic benefits of correcting near-vision impairment (presbyopia) in adults.
The five-year study will look specifically at adults ages 35 to 65 with presbyopia by running two randomized controlled trials in India and Kenya. With 20,000 patients to be engaged across two countries, participants will either receive reading glasses at the outset or be placed in a control group without them, with the latter group receiving glasses at the end. The investigators will collect data at baseline, then one and two years in, to evaluate the impact that having – or not having – glasses has had on participants by looking at household spending, quality of life, employment, work productivity and income.

Operation Eyesight’s role is to identify patients to enrol in the study in Kenya – and to continue managing patients with other eye health problems that don’t meet the parameters of the study. Participants will be selected from Kisii County, where we’re already running community eye health programs.
Senior Program Manager Edwin Wanjala Simiyu is overseeing Operation Eyesight’s participation in the study.
“Operation Eyesight was selected to work on this study because of our historical engagement with Peek Vision, with whom we’ve successfully implemented several projects,” he explains, referring to our longtime partner who created the eye health technology that will be used to gather data for the study.
He adds that the study is helping us foster important new collaborations. “Partnerships bring on board new ideas that shape project implementation and impact. It also reduces the project unit cost due to shared responsibilities.”
Gathering evidence on the effectiveness and economic impact of eye health treatments – such as a simple, low-cost pair of reading glasses – helps us demonstrate to decision makers how they can improve lives and livelihoods through cost-effective solutions.
Using our insights to advocate for eye health care
Members of our international team are frequently invited to sit down with various government agencies to offer their knowledge – sharing lessons hard-learned through years of program delivery.
In Kenya, while focusing on the Universal Eye Health Coverage agenda, we worked with the ministry of health to review the World Health Organization’s Primary Eye Care Training manual to better standardize primary eye care delivery nationwide, while in Ghana, we participated in a joint press conference hosted by that country’s ministry of health ahead of World Sight Day.
In addition, we are increasingly being called upon to act as technical partners, where we share our expertise on creating and managing sustainable eye health programs. Over the past few years, our team in India has worked closely with the health ministries of state governments in Arunachal Pradesh, Madhya Pradesh and, more recently, Meghalaya to establish vision care facilities within already-existing government health centres, such as Health and Wellness Centres.
Now, we’re looking to spread awareness in Canada, where our head office is located, though our involvement in the National Strategy for Eye Care Act. The act, passed in November 2024, aims to provide equal access to eye health care services across Canada and to improve the prevention, treatment and rehabilitation of eye conditions for all.

In Canada, vision care is covered by a complex framework of provincial and federal regulations, meaning that coverage varies widely between provinces and territories. For routine vision care – like eye exams and prescription eyeglasses – many Canadians need to pull from health insurance to cover the costs. Those who are uninsured may have to pay out of pocket. These inequities are what the act proposes to address.
Now, as the chair of the Canadian Eye Health Coalition, Operation Eyesight is helping shape the framework for the national strategy. That means meeting regularly with like-minded partners and policymakers to continue the important work of making eye health care more equitable and accessible across the country.
Global Director Kris Kelm says that we’re well poised to inform decisions because of our decades of experience delivering sustainable eye health programs.
“We have the opportunity to shape what the developing policy is going to look like and how it’s actually going to affect Canadians,” he says. “As a non-profit dedicated to eye health and ensuring equitable access for all – regardless of socioeconomic status – it’s critical that we’re part of the conversation.”
Operation Eyesight is also a proud member of IAPB, adding to the collective, global voice advocating for the prioritization of eye health. Next year, we will participate in the first ever Global Eye Health Summit, which will bring together governments, organizations and the private sector to foster collaboration and mobilize action.
As we continue to collect data from communities around the world, we’re not just measuring outcomes, we’re helping to shape them. Every survey completed and every study published brings us closer to a world where quality eye care is accessible to all.
Whether it’s through national studies, local program evaluations or global research collaborations, we remain committed to using data as a tool for change. As we keep pushing for fair and accessible eye health care around the world, we’re proud to build on the knowledge and trust we’ve earned from the communities we work with. After all, they’re the reason we do what we do – For All The World To See.
At age 70, Saidur in Bangladesh continues to work on his farm to support his large, extended family. He knows that without his income, his family’s finances would be spread too thin.
But in recent years, farming became increasingly difficult for Saidur as his vision weakened. “It was as if everything had turned dark and blurry,” Saidur recalls. Eventually, his eyesight became so bad that he could no longer work at all. He felt helpless, stuck at home, worrying about the family’s future.
When a community health worker showed up on the family’s doorstep, announcing that she would examine the family’s eyes, Saidur felt the first stirrings of hope. When it was his turn for a screening, the health worker quickly identified him with bilateral cataracts. She explained to him that treatment was available at our partner facility, the Dr. K. Zaman BNSB Hospital in the nearby city of Mymensing, and that he could get the surgery free of charge.

The idea of travelling to the city for surgery was daunting to Saidur, who had never undergone an operation before, but encouraged by the support of the community health worker and his family, he decided to take the leap and committed to getting it done.
After his cataract diagnosis was confirmed at the nearby Madarganj Vision Centre, which we helped establish in partnership with Symbiosis International, Saidur travelled to Mymensingh for his surgery. When the bandages were removed, he was amazed by the results. The world was once again vivid and clear, and he felt the burden of his worries lifting. He received a pair of eyeglasses to further correct his vision, and he soon returned to his farm work – his independence and sense of purpose restored.

After that, Saidur found himself telling anyone who asked about his miraculous transformation. “I’ve already referred at least seven to eight people with eye problems to the vision centre,” he says proudly. “If anyone in my community has vision issues, I will personally take them there.”
Saidur credits the dedication of the community health worker and the team at Dr. K. Zaman BNSB Hospital for their compassionate care, and he is grateful for the financial support for the surgery. “Their care and kindness were beyond measure,” he adds. “I’m very happy to be able to see my grandchildren.”
Now, with his vision restored, Saidur is filled with gratitude and determination to help others access the same life-changing care.
Donate today to help us prevent blindness and restore sight in more people like Saidur.
If you sprain an ankle or come down with a bad cough, your first stop is usually your family doctor. But when it comes to blurry vision, the path to care often looks very different. Around the world, eye health is still treated separately from primary health care, creating gaps that leave people without the vision help they need. Even in countries with universal health coverage, you might receive a complex eye surgery at no cost, yet pay out of pocket – or use private health insurance – for something as simple as a pair of eyeglasses.
At Operation Eyesight, we believe this needs to change. That’s why we’re working to strengthen areas of overlap between primary eye care and primary health care in our countries of operation. That means supporting the World Health Assembly’s integrated people-centred eye care (IPEC) resolution by working to integrate eye health into national health systems – and increasing access to free or subsidized eye health care.
It also means addressing the root causes of avoidable vision loss. In some regions in Africa, we bring fresh water and hygiene education to communities to help prevent infectious eye conditions. We also work to make sure our services offer more than just eye care, but can also link patients to other types of health care.
Health conditions rarely exist in silos – and vision loss is no exception. Diabetes, for example, increases the risk of eye conditions like cataracts. For 15-year-old Vanessa in Zambia, blurry vision was one of the first signs of the disease. When she started having problems reading the blackboard at school, a teacher sent her to our vision centre in her community of Matero for a checkup. From there, she received a referral to our partner hospital, where she learned that she not only had cataracts, but diabetes as well. Doctors helped her get her blood sugar levels under control, and then she got cataract surgery. Today, she is managing her diabetes and thriving in school, with dreams of becoming a doctor.

Vision problems can also cause a downward mental health spiral. Benson, a farmer in Kenya, lost his ability to work due to poor vision. As a result, he became angry and depressed, then turned to alcohol and drugs to cope with his situation. Luckily, his family got him into a drug and alcohol rehabilitation facility, where a visiting doctor diagnosed him with cataracts. Benson underwent surgery on both eyes, provided free of charge thanks to the support of our donors, and can see clearly now. Buoyed by his miraculous recovery, Benson finished up his time at the rehabilitation facility and happily threw himself back into farming.
In Canada, where Operation Eyesight is based, navigating eye care can be confusing. While the Canada Health Act covers medically-necessary eye health services, routine vision care like eye exams and prescription glasses often isn’t part of the deal. That leaves provinces and territories to fill in the gaps, and the result is a patchwork system. For example, seniors in Ontario get routine eye exams covered once they hit 65, but in Newfoundland and Labrador, those same seniors might have to pay out-of-pocket. It’s inconsistent, and it’s especially tough on vulnerable populations.
There is some support through the Federal Non-Insured Health Benefits (NIHB) program, which covers eye exams and eyewear for eligible First Nations and Inuit individuals. But even that has its hurdles: remote communities, limited healthcare infrastructure and cultural differences that make accessing care more complicated than it should be.

The passage of the National Strategy for Eye Care Act in 2024 was a major step forward in addressing these issues. As chair of the Canadian Eye Health Coalition, Operation Eyesight is helping shape a national framework that prioritizes equitable access to vision care. Our Global Director of International Programs, Kris Kelm, explains why it’s important that we have a seat at the table during the consultation period and beyond.
“We know that there will be many voices in this conversation with diverse interests, and we want to ensure there is representation from patients who have the least means and the least ability to access vision care,” he says. “The fact that we have over 60 years of experience working in this sector gives us a strong background to speak credibly to how we need to approach things in Canada, and our community partners can provide valuable insights to help shape eye care for all.”
He adds that Canada can learn from some of our countries of work, where eye health has been better integrated into the overall health systems and other public frameworks. As an example, he points to Ghana, where we work with the ministries of health and education to screen and treat students for eye conditions in the public school system. We have similar programs in Kenya and Zambia, too.
Another example is in India, where we are working with state governments to establish vision services in pre-existing government health centres. Building the capacity of vision care facilities within the country’s national health care system ensures that services reach the most underserved populations, as patients who are able to pay most typically seek care at for-profit facilities, rather than attending government services.
Shakuntala, in Madhya Pradesh, India, spends her days walking door to door through villages in her region, checking in on the health and well-being of families. She’s one of the million-strong network of Accredited Social Health Activists (ASHAs), employed by the Indian government, who deliver primary health care at the community level.

Her work includes providing pregnancy advice, supporting newborn care, educating parents about vaccinations and vitamins for children, and making all kinds of referrals to local clinics and hospitals. In 2022, Shakuntala added another set of skills to her toolkit: conducting primary eye health screenings, thanks to training provided by our Operation Eyesight team, in partnership with the Government of Madhya Pradesh. Shakuntala learned to measure visual acuity using an eye chart. She also learned to identify the signs and symptoms of various eye conditions. Once she identifies a patient with a possible eye condition, she refers them to the base hospital for diagnosis and treatment. In the meantime, she continues to provide advice and referrals on nutrition, vaccinations, prenatal care and other health concerns.
Shakuntala is just one of the thousands of community health workers we work with across the globe. In all our countries of work, we partner with existing health systems to recruit community health workers, mostly women, to help us deliver our programs. The health workers develop strong ties within the communities, resulting in high acceptance and trust in our programming.

Mabel, a community health nurse in Ghana, was trained in primary eye care so that she could identify eye health issues in addition to her regular duties. She says that being able to screen people at their home allows her to reach many women and girls who probably wouldn’t have left the village to seek eye health care, due to household responsibilities.
Anyone who has had a case of pink eye knows that having red, inflamed and itchy eyes isn’t much fun. But in some parts of the world, an eye infection can be a much more serious problem. Trachoma is an infectious eye disease that leads to vision loss and blindness in millions of people across the globe. It spreads easily through contact with eye discharge from infected people on hands and clothing, and through flies. If left untreated, chronic infections turn the eyelid inwards, causing intense pain and scarring of the cornea, which can lead to irreversible blindness.
Trachoma is preventable, and clean water is key to curbing the spread. When communities have access to clean water, people can clean their hands, faces and clothing more often, which prevents it from spreading.
In countries like Zambia, we work with Water Affairs (the government department responsible for water) to drill, rehabilitate and repair boreholes near where people live, work and go to school, so that whole villages have access to clean water. We also provide training to local volunteers in these communities in WASH (Water, Sanitation and Hygiene) and borehole repair and maintenance to ensure the clean water continues to flow. In areas where trachoma is endemic, we also work with partners to distribute antibiotics, which both treats and prevents trachoma.

It's another way that we work to address one of the root causes of avoidable vision loss, but it also helps us tie into improved health outcomes overall. Accessible clean water helps prevent dozens of infectious diseases. It also improves quality of life for women and girls, who are often tasked with the job of fetching water, which can take up hours out of the day and prevent them from participating in school, work or other activities. Moreover, clean water means people can grow vegetable gardens, raise livestock and keep entire families, and communities, happier and healthier.
When we invest in sight, we invest in education, productivity and dignity. To eliminate avoidable vision loss, vision care needs to be recognized as a public health priority and integrated into national health strategies. Operation Eyesight’s global experience – from rehabilitating boreholes in Zambia to collaborating with partners on new policies in Canada – demonstrates that integrating eye health into primary care, addressing environmental determinants like access to clean water, and empowering community health workers leads to sustainable, measurable outcomes. Policymakers have a critical role to play in building resilient health systems that ensure equitable access to vision care for all.
Read more about our approach to Hospital-Based Community Eye Health.
At 13 years old, Erasmus is like many other boys his age: tall, gangly and a little bit shy. He says he’d like to be a soldier when he grows up.
While joining the military seems achievable, that dream was nearly shattered for Erasmus a few years ago, when an accident threatened both his vision – and his future.
It all started one evening back in 2019. Erasmus’ mother, Joyce, was inside their home in the rural community of Essiam, in Ghana’s Central Region, when she suddenly heard shouts coming from outside, where Erasmus was playing with friends. She rushed outside and found her son clutching his eye in pain. His friends told her that something had flown through the air and hit him hard in the eye.
Initially, Joyce treated Erasmus at home with some over-the-counter eye drops, but after going to school the next day, he said he was still feeling a lot of pain. His teacher recommended Joyce take him to the hospital to get it checked out.
Joyce took him to the nearest hospital, and the doctor there referred them to the Korle Bu Teaching Hospital in the capital city, Accra. He also advised her to make sure that nothing happens to Erasmus’ other eye, as he worried that the boy might lose sight entirely on the injured side – advice that shook Joyce to the core. She imagined her son’s future melting away, along with his eyesight.
As a single mother running a small hair-braiding salon, Joyce was overwhelmed by the cost and logistics of travelling to Accra. Eventually, she got some money together and they went to the hospital. A doctor examined Erasmus and told Joyce the damage to his eye was very serious and that he would need surgery.
But Joyce couldn’t afford the surgery. She tried everything – asking family for help, borrowing what she could – but it was never enough.
In the meantime, Erasmus continued to have pain and irritation and couldn’t see much out of the affected eye. Joyce, tears spilling from her own eyes as she remembers that bleak period, says she was terrified for her son and felt completely alone in dealing with the problem.
Then, in 2023, she learned that a charity had visited Erasmus’ school and had checked on the students’ eyes. She rushed down to the school and learned that Erasmus had been identified as a student in need of a referral for a more thorough diagnosis.
That eye charity was, of course, Operation Eyesight, working in tandem with the ministries of health and education, and our partner hospital, Watborg Eye Services, in Awutu Breku. Erasmus got a referral to Watborg, where he received a thorough eye exam.
Joyce learned that her son’s injury had developed into a cataract. A traumatic cataract happens when an eye injury disrupts the lens fibers – leading to a clouding of the lens. Up to 1.6 million people lose sight to eye injuries each year.
Erasmus was scheduled for surgery in two weeks’ time. And although Joyce was told that the surgery would be provided free of charge, she couldn’t quite believe it and continued to worry about the costs.
Two weeks later, Joyce and Erasmus returned to Watborg for the cataract surgery. Doctors told her the operation went well, and they kept Erasmus in hospital for another couple days to allow the eye to heal.
To Joyce’s relief, she learned that the surgery was in fact done free of charge, made possible through our School Eye Health Project supported by the Church of Jesus Christ of Latter-day Saints Charities. The project covered all other expenses, including transportation, meals, the hospital stay and post-surgical appointments.
Due to the complexity of Erasmus’ injury, it would take him additional time to recover than most cataract patients. For weeks after the operation, Joyce anxiously asked, “Can you see yet?” The answer was always no — until one day, Erasmus burst into her salon shouting, “Ma, I can see! I can see!”
Erasmus now wears prescription glasses to school, his future once again in focus. Joyce, deeply moved, says she’s forever grateful to Operation Eyesight and our partners for restoring her son’s sight, and her hope.
As always, we are gearing up for a variety of World Sight Day events, including eye screenings, awareness marches and more. The global celebration is an opportunity to spread awareness about the importance of eye health. It’s also a chance for us to stand with our partners to call on policy makers all over the globe to make eye care accessible and affordable for everyone by providing universal health care that includes eye care.
This year, get your youngest family members involved by participating in our World Sight Day Wellness Bingo, an activity that challenges kids to take care of their eyes. Download your copy today.
In November 2024, the Canadian federal government passed the National Strategy for Eye Care Act. As a member of the Canadian Eye Health Coalition, we are proud to chair this network of organizations and individuals working together to inform the national framework for eye care and advocate for improved vision health for all Canadians.
When I first met Mary*, she told me how she had been blind since 2012. She had started losing her vision when she was very young – when she was a new bride and expecting her first child. Living in a rural area, far from any hospitals, she went to a traditional healer for help but continued to lose her sight. People whispered that she must have been doing witchcraft that backfired on her… asking what else could explain blindness in someone so young. Believing the witchcraft rumours, Mary’s husband left her before the baby was born. Her family abandoned her too. The only person who helped Mary was her niece, who has been supporting her and her child all this time.
When the niece heard that Operation Eyesight was offering free eye exams, she brought Mary to a surgical camp we were hosting. After all her years of alienation, Mary had little confidence in getting her sight restored, but she agreed to a checkup in hopes that it would reduce the eye pain she was experiencing. The team diagnosed her with bilateral cataracts and recommended surgery, which she agreed to.
I went to check on her in hospital shortly after her bandages came off. I was initially disappointed because she kept saying, “No, I can’t see you. I can't see anything.” Worried something had gone wrong with the operation, I called her over to see the doctor, when she finally said, “Actually… I can see you, but I’ve been blind for so long, I thought I was imagining you! I’ve been able to see you the whole time.”
She erupted into laughter, then tears. Her niece joined in.
We escorted her home by public bus, and the whole time she was pointing and smiling at things she saw rushing by through the window. She said her greatest excitement was seeing the face of her daughter – now 12 years-old – as soon as she got home.
*name has been changed to protect the patient’s privacy

Candy Siadibbi joined our Zambia team in 2022, first working in the Lusaka area before relocating to Mkushi, in Central Province. She has a bachelor’s degree in psychology and public administration from the University of Zambia. Before joining Operation Eyesight, she worked as a research assistant, freelancing with various nonprofit organizations.